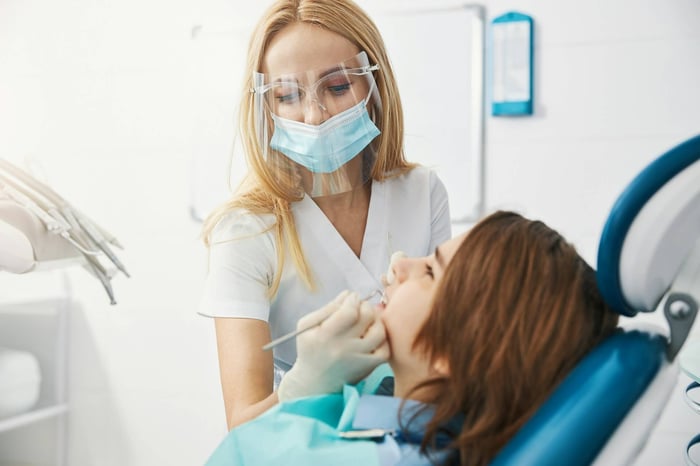
Hearing that you may need a molar tooth extraction can feel a little intimidating at first. The good news is that removing a damaged or infected molar is a common dental procedure that often relieves pain and protects the rest of your teeth.
At Care Dental Center, molar extractions are carefully planned to remove the problematic tooth while ensuring a smooth and comfortable procedure. Modern dental tools and precise imaging help dentists remove molars safely while protecting nearby teeth and bone.
In the sections ahead, we’ll walk through why a molar sometimes needs to be removed, what actually happens during the procedure, and what recovery usually looks like in the days after treatment.
Why Molars Sometimes Need to Say Goodbye
Molars can cause pain, bite trouble, and even infect nearby teeth. Taking out a molar can stop infection, protect others, and help your mouth work better.
Common Reasons for Removing a Molar
When decay reaches deep inside, and a filling or crown can’t fix it, you may need a molar pulled.
Deep cavities that hit the nerve usually bring constant pain and can cause an abscess. Dentists often pick extraction over a root canal if the tooth is badly broken, previous treatments failed, or if cost and long-term outlook make other options unrealistic.
Sometimes, crowding or orthodontic plans mean a molar needs to be removed to make space for straight teeth.
If a molar sits too high or tilts, chewing might suffer—removal can improve your bite. After extraction, the dentist will talk about replacement choices like an implant or bridge to make chewing easy and prevent teeth from shifting.
Wisdom Teeth and Their Unique Challenges
Wisdom teeth usually show up late and can get stuck under the gum or the bone. Impacted wisdom teeth might swell, hurt, cause bad breath, or spark an infection. They sometimes damage the second molar by wearing down its root or trapping food and bacteria.
The dentist checks the position and root shape with X-rays. If things look tricky, you might get local anesthesia, sedation, or a referral to an oral surgeon. Removal gets recommended when keeping the tooth risks your oral health more than taking it out.
Recovery after wisdom tooth removal usually means some swelling, a soft-food diet, and basic home care.
Periodontal Disease and Your Molar Health
Gum disease can loosen a molar by destroying the bone that holds it in place. If deep pockets of bacteria form, cleaning and antibiotics might not save the tooth. You could notice bleeding gums, loose teeth, or a bad taste that lingers—clear signs of active periodontal disease.
When bone loss gets severe, extraction helps stop the spread of infection and shields nearby teeth.
After a molar comes out for gum reasons, you’ll focus on treating your gums—scaling, root planing, and better home care—to keep other teeth healthy. Newer tools and gentle techniques make the process more comfortable and predictable.
Preparing for Your Molar Extraction Appointment
Learn what images and exams the dentist uses, which anesthesia options you might get, and what health info you should share with the team. These steps help prevent surprises, shorten your visit, and keep you safer during the procedure.
The Role of Dental X-Rays and Exam
Dental X-rays show where the molar sits, how its roots look, and what’s nearby. The dentist or oral surgeon takes a panoramic or periapical X-ray to check for impaction, root shape, and nerve location. This planning helps decide if you need a simple extraction or oral surgery.
During the exam, the provider checks gum health, mouth opening, and nearby teeth. They’ll talk through findings and explain the plan. If you have recent dental records or X-rays, bring them; it makes things go faster.
Anesthesia Options: What Will You Feel?
Local anesthesia numbs the area around the tooth. You’ll stay awake and might feel pressure, but not sharp pain. The shot can sting for a second, then the area goes numb quickly.
If the tooth is impacted or removal is complicated, sedation or general anesthesia might be on the table.
Nitrous oxide (laughing gas) helps you relax but keeps you awake. IV sedation or general anesthesia makes you drowsy or puts you out; an oral surgeon usually handles these. The team explains risks, fasting rules, and recovery time for each option so you know what’s coming.
What to Share with Your Dental Team
Let the team know about all meds, including blood thinners, aspirin, and herbal stuff. These can affect bleeding and healing. Also mention medical conditions like diabetes, heart issues, or immune disorders.
Tell them about allergies, recent illnesses, and any past problems with anesthesia. Share if you’re pregnant or breastfeeding. If you’re nervous, say so; they can offer sedation options and calming tips. Give contact info and arrange a ride home if you’ll get sedation or general anesthesia.
How the Extraction Actually Happens
Here’s what separates simple and surgical removal, what the team does step by step, and how they keep you as comfortable as possible during and after a molar extraction.
Simple Extraction Versus Surgical Extraction
For a simple extraction, the dentist numbs the area and uses forceps to rock the tooth free. This works for most molars that have erupted normally and have a solid crown above the gum.
A surgical extraction gets a bit more complicated. The dentist or oral surgeon makes a small cut in the gum, may remove some bone, or splits the tooth into pieces to take it out safely. Heavier sedation, like nitrous oxide or IV sedation, might be needed if anxiety or tooth position calls for it.
Share your medical history and meds before either type. That helps the team choose the right anesthesia, lowers bleeding risk, and helps with healing.
Step-by-Step Walkthrough of the Procedure
First, you’ll get local anesthesia to numb the tooth and gum. The dentist checks numbness before starting, so you’ll feel pressure but not sharp pain. For simple cases, the dentist loosens the tooth with elevators and lifts it out with forceps.
They clean the socket and place gauze to form a clot. For surgical cases, the dentist makes a small cut, may remove bone, and might section the tooth for easier removal. Stitches often go in if the gum gets cut.
The visit usually takes 20–60 minutes, depending on how tricky things get. The team explains aftercare, like biting on gauze, avoiding rinsing for 24 hours, and how to use any prescribed meds.
Managing Discomfort and Staying Comfortable
Expect soreness and mild swelling for a few days. The team gives pain-relief tips, usually recommending over-the-counter painkillers or prescribed meds if needed. Stick to the dosing schedule.
Try ice packs on your cheek for the first 24 hours to keep swelling down. Eat soft foods and skip straws or spitting for 48 hours to protect the clot. Keep your head up while resting and gently clean your mouth after 24 hours.
If pain gets severe, bleeding is heavy, or swelling gets worse, call the office right away. The team can help manage any issues that pop up.
Healing, Recovery, and Your Life After Extraction
Bleeding, swelling, and soreness are normal at first. Follow the steps to control bleeding, ease pain, and keep the socket safe for smoother healing.
Immediate Aftercare: Stopping Bleeding and Swelling
Bite gently on a clean gauze pad for 30–45 minutes to form a clot. If bleeding keeps up, swap the gauze and keep pressure; don’t spit or rinse for the first 24 hours. Use an ice pack on your cheek for 10–15 minutes on, then off, during day one to cut swelling.
Keep your head up when you rest. Take pain meds as directed—either prescribed or over-the-counter ibuprofen. Skip aspirin because it can increase bleeding. Drink cool fluids and eat soft foods like yogurt or mashed potatoes for a few days.
Avoiding Dry Socket and Other Complications
Dry socket happens when the blood clot comes out, and sharp pain hits a few days after extraction. Don’t use straws, smoke, or spit hard for at least 72 hours to protect the clot.
Brush gently and avoid the extraction site until your provider says it’s okay. If you need to rinse after 24 hours, use saltwater (1/2 teaspoon salt in 8 ounces of warm water) gently a few times a day.
Watch for infection signs: more pain, bad taste, fever, or swelling. If you suspect dry socket or infection, call the office for help.
Long-Term Options: Implants, Bridges, and Dentures
If you lose a molar for good, you can get a dental implant, a fixed bridge, or a removable partial denture. Implants replace both root and crown and help keep your jawbone healthy, but the process takes months.
A bridge uses nearby teeth as anchors and restores chewing pretty quickly, but it might affect those teeth over time. A partial denture is removable and often a more affordable way to restore function and appearance.
Talk timing with your dentist; sometimes the socket needs to heal before an implant or bridge goes in. The team explains each option, the costs, and the steps so you can pick what fits your life.
Why Replacing A Missing Molar Often Helps Long-Term Oral Health
Replacing a missing molar helps maintain balance in the bite. According to MedlinePlus, gaps left by missing teeth may cause nearby teeth to shift over time.
These shifts can affect chewing and may change how upper and lower teeth meet. MedlinePlus explains that tooth replacement options like implants or bridges help maintain alignment and restore chewing ability.
Planning replacement with your dentist helps protect the surrounding teeth and keep your bite functioning properly.
Tips for a Smooth Recovery at Home
Rest for 24–48 hours and skip heavy lifting or tough exercise for a few days. Stay hydrated and eat soft, healthy foods to help with healing. Avoid hot drinks, alcohol, smoking, and hard foods that could bother the socket.
Use a straw only when your dentist says it’s okay. Keep your follow-up visits so the provider can check healing and remove stitches if needed. Brush gently, avoid the extraction site, and rinse as instructed to keep your mouth healthy.
When A Molar Needs To Go, The Right Plan Makes It Easier
A molar tooth extraction is sometimes the best way to stop pain, remove infection, and protect the rest of your teeth. With careful planning and modern techniques, the procedure is usually quicker and more manageable than many people expect.
At Care Dental Center, molar extractions remove damaged teeth to ensure smooth recovery and protect long-term oral health. Clear explanations and thoughtful treatment planning help patients feel more confident about the process.
If you’ve been told a molar may need to be removed, a dental evaluation can help you understand your options and plan the next steps for healing and tooth replacement.
Frequently Asked Questions
This section covers common concerns about pain, costs, risks, and healing after a molar extraction. You’ll get straightforward answers to help you plan and feel less stressed.
What are some common side effects I might experience after molar extraction?
You might have bleeding for a few hours and mild swelling for 2–3 days. Soreness in the jaw and at the extraction spot can last up to a week. Minor bruising, jaw stiffness, and a temporary bad taste are pretty normal. If numbness lasts past a few hours or you have heavy bleeding, call your dentist.
Can you explain the advantages and potential drawbacks of removing a lower molar?
Taking out a damaged lower molar stops infection and pain. It also keeps nearby teeth from shifting and can make future care simpler. Drawbacks are short-term pain, swelling, and less chewing on that side while you heal. Rarely, lower molar removal can affect the nerve to your lip or chin; your dentist will discuss this risk.
How much does it typically cost to have a molar tooth removed?
Simple extractions usually cost a few hundred dollars. Surgical or impacted extractions often run higher, sometimes several hundred to over a thousand dollars. The price depends on how complex the case is, x-rays, anesthesia, and insurance. For an estimate or to ask about payment, just reach out to the office.
What are the possible complications associated with upper molar extractions?
Upper molars sit near the sinus, so sometimes a small opening into the sinus happens during removal. Usually, these heal on their own, but occasionally, they need a follow-up repair. Other risks are infection, bleeding that won’t stop, or slow healing. The dentist checks your sinuses and explains how to reduce risks before starting.